 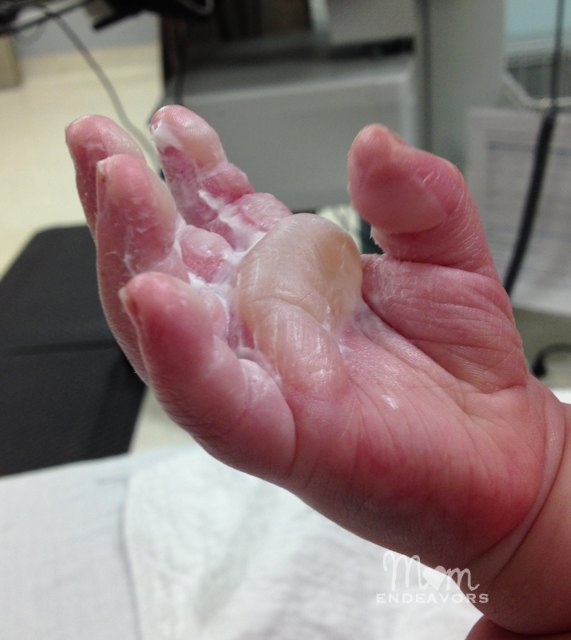 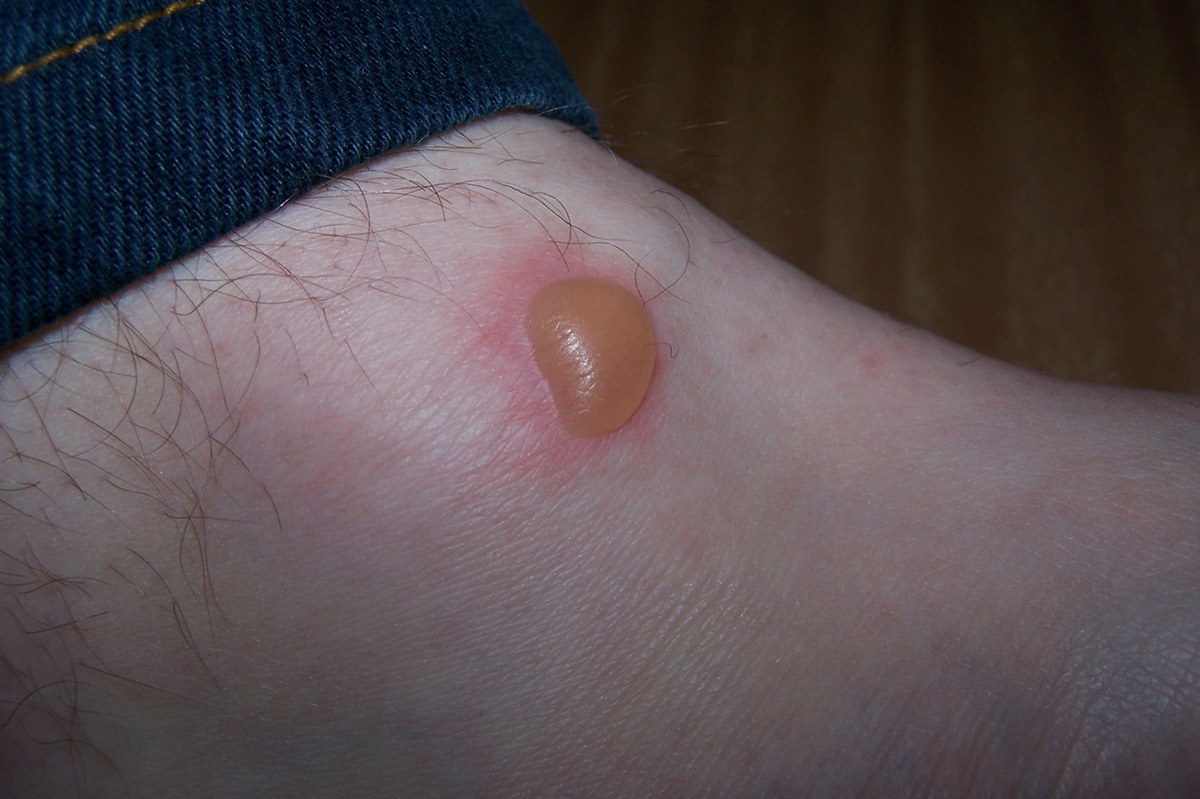
When thinking about burn debridement, there are really two separate (but related) questions. Their conclusion is “based on the current available evidence, blisters should, wherever possible, be left intact to reduce the risk of infection, but if anatomical position necessitates intervention for functional purposes, aspiration appears to result in less pain than deroofing.” (Shaw 2006) There is a BestBET review on this topic from 2006, and the only paper they found that matched their search criteria was the paper by Swain. However, scarring was worse at all timeframes in the debridement group, based on a validated scale. There were no major differences between the groups. It wasn’t a perfect study, with no blinding of physicians or patients, and inadequate allocation concealment (they used a coin flip). This study doesn’t help us a lot, because they didn’t include a control group where they left the blisters intact. Ro (2018) studied 40 patients with burn blisters and randomized them to their aspiration or deroofing of the blister. Colonization is not really a patient important outcome, and they don’t report the rate of infection here. There was a much higher rate of bacterial colonization in the aspiration and deroofing groups (70% and 76% vs 14%). All patients healed well with conservative management. Burn blister trial#Swain (1987) performed a non-randomized, open label trial where 316 patients with partial thickness burns had their blisters left intact, aspirated, or debrided. Of course, there is no way to know that the burns were equal to begin with, and this is a single patient. The right leg (no debridement) had less pain, faster healing, and better cosmetic results at 1 year. They left the blisters in tact on the right and debrided the left. They decided to use the legs as their own controls. Healing rates seemed to be slower with aspiration and debridement.įorage (1962) presents a case report of a 14 year old girl with burns to both of her legs. The numbers are small, but the only group whose wounds were 100% healed by day 14 was the group with their blisters left in tact. On each “volunteer” they made 12 to 16 one centimeter burns across the abdomen, which after blister formation were either left in tact, aspirated, or debrided (at various different timeframes). Gimbel (1957) is a fascinating study in that they purposefully burned medical student volunteers. (Which unfortunately leaves us with very little to look at.) Therefore, I will only look at clinical studies. They care about pain, speed of healing, scarring, and function. (For a nice overview, see Flanagan 2001) More importantly, patients don’t care about the thromboxane levels in their blister fluid. When it comes to burn management, it is basically impossible to make a decision based on physiologic reasoning, because different experts make different recommendations based on the same data. I am always wary of basing clinical decisions on physiologic studies, because they have been wrong too often in the history of medicine. There is much theoretical debate about the various biochemicals contained in blisters, and whether they are bad or good. (Sargent 2006) Reviews of this topic spend most of their time discussing physiologic data and animal models. 
Given that practices vary drastically from hospital to hospital, no one treatment strategy can be considered standard care. (Spoiler: there aren’t.)Īlthough there are many strong opinions, there are no definitive answers. Given the clear downsides of this new practice, I thought it would be worthwhile to review the evidence, assuming there must be some new high quality studies that prompted this advice to debride burn blisters. 
Although I love procedures, the referred patients are almost always small children, who require sedation, with difficult IV access, and end up occupying a much needed ED bed for a long period of time. It was also recommended on a fantastic episode of Emergency Medicine Cases. Both in Canada and New Zealand, I have had plastic surgeons refer patients back into the emergency department to have their burns debrided. Recently I have noticed a push to have burns debrided. My teaching was to leave the blisters alone, as deroofing them provides no benefit but increases pain. The management of burn blisters has always produced a lot of debate. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
